Dr. Leonardi Discusses Advancements In Imaging For Endometriosis And Diagnostic Care

Dr Mathew Leonardi is an expert in complex gynecology, endometriosis excision surgery and gynaecological ultrasound (associate professor) at McMaster University Medical Centre in Hamilton, Canada. He is an honorary adjunct lecturer at the University of Adelaide. His philosophy of care includes working in an interdisciplinary team and patient-centred decision making. He has been awarded his PhD from the University of Sydney which is focused on the utility of ultrasound in the diagnosis and surgical management of endometriosis.
Dr Leonardi is a nationally and internationally recognized leader in his field. He has published over 120 peer-reviewed scientific articles, several textbook chapters, and presented at numerous international congresses on endometriosis. He has received numerous awards for his conference presentations on endometriosis. He is an avid researcher, actively contributing academically to the advancement of gynecologic health.
Dr. Leonardi is on the World Endometriosis Society Early Career Board and a founding member of the Next Generation Committee at the International Society of Ultrasound in Obstetrics and Gynecology. He is an Associate Editor for Reproduction & Fertility and on the Editorial Board for the Journal of Minimally Invasive Gynecology, Ultrasound in Obstetrics and Gynecology, and the Journal of Obstetrics and Gynaecology of Canada. He is part of an international research group named Imagendo, which won the most prestigious science award in Australia, the 2023 ANSTO Eureka Prize for Innovative Use of Technology.
He believes in listening to patients, validating their experiences, and working together with the patient to achieve the best outcomes. The Endometriosis Network Canada (TENC) spoke with Dr. Leonardi about his exciting work and its implications for patients.
The Endometriosis Network Canada (TENC): Thank you so much for speaking with us today! To start, can you tell us about what are the different types of imaging that are used for people with endometriosis or suspected endometriosis, and how they are helpful?
Dr. Mathew Leonardi (ML): When someone experiences the symptoms of endometriosis, we should be utilizing a comprehensive imaging approach to these patients. There are two broad imaging modalities currently used to assist in diagnosing endometriosis: ultrasound and magnetic resonance imaging (MRI), both of which require expertise to perform and interpret.
Right now, there is a standard of care ultrasound in Canada, as per the Society of Obstetricians and Gynaecologists of Canada and the Canadian Association of Radiologists. This ‘basic pelvic ultrasound’ looks at the uterus and the ovaries. We also sometimes look for fluid in what we call the cul-de-sac, or the rectouterine pouch (Pouch of Douglas). That is the extent of it, which means that an ovarian endometrioma – one of three types of endometriosis – can be identified and diagnosed. The other two phenotypes of endometriosis – deep endometriosis and superficial endometriosis – cannot be identified and diagnosed using this method.
The advanced pelvic ultrasound goes significantly further than the basic pelvic ultrasound to look outside of the uterus and the ovaries. It looks at the front compartment of the pelvis (bladder and the ureters), and the rear compartment, which includes the bowel, the uterosacral ligaments – the most common site of endometriosis – the rectovaginal septum, the torus uterinus, and the rectouterine pouch. This ultrasound has the ability to diagnosis deep endometriosis. It can also diagnose adhesions in the pelvis, as it utilizes dynamic movements to understand how the pelvic organs move together or don’t.
The group that is inspiring the new ultrasound is called the International Deep Endometriosis Analysis Group (IDEA), and I encourage everyone to check out their recent publication for more information.

TENC: What are some of the limitations with imaging?
ML: There are a few. We spoke about two of the three subtypes of endometriosis; ovarian endometriomas and deep endometriosis. The remaining subtype is superficial endometriosis. This type is quite small, difficult to see, and often flush with the peritoneum (the lining of the pelvis). Right now, the people in the world who are doing advanced ultrasound for endometriosis are not routinely looking for superficial endometriosis because it is very challenging, and likely they haven’t yet been instructed on exactly how to do that.
One of my main areas of research as part of my PhD under the supervision of Professor George Condous in Sydney, Australia is to understand how ultrasound can diagnosis superficial endometriosis.

We use a technique that is similar to what we call a sonohysterography. This is an ultrasound where we put fluid into the uterus. If the fallopian tubes are open, the fluid will travel through them and into the pelvis. The fluid fills the cul-de-sac and allows the structures around the pelvic peritoneum to move away. As it moves the bowel and structures apart, you can see subtle features like this a little more easily.
“The other big limitation – and this is glaringly obvious to endometriosis sufferers in general – is expertise.”
We speak about the need for endometriosis experts. Right now, most of that discussion is surrounding the actual treatment of endometriosis. We need endometriosis experts who are experts in the diagnosis and treatment of the disease. Most imaging specialists in the world are radiologists, who take a broad training program that includes all parts of the body and all disease types, so very few are subspecialized in the intricacies of endometriosis. As such, expertise in radiology for endometriosis is limited. Expertise amongst OBGYNs for imaging is also very limited as it’s not part of the training.
TENC: Wow, that expertise would be life-altering for so many.
ML: Absolutely! It’s so important for people to understand their condition, not just how to manage symptoms. This is why I pursued a combined fellowship in both imaging and surgery, to address this major gap and return to McMaster University to share what I’ve learned and hopefully change the future of endometriosis diagnosis and treatment.
TENC: Where do you envision the role of imaging in diagnostic procedures and standards for endometriosis five years from now?
ML: Very difficult question to answer. Five years in medicine is not a lot of time. Unfortunately, things do not change very quickly because there are many factors that go into advocating for change and then implementing change. In five years we will have trained several additional fellows in Canada – at least in the program at McMaster, and there are several other programs in the country that are already implementing advanced imaging for endometriosis including UBC and the University of Ottawa. Progress is slow, but it’s still progress!
One of my strategies is to engage with the endometriosis community directly because for a long time the community has driven change. I recognize this, and we must use this motivation and work together. If we educate patients, patients can educate their doctors. And while that is not how it should be, it is the reality, so have to do our best to work together to improve the state of things. So, in five years, I think we are going to be better than we are now, but that there is still to be a hill to climb; there is still going to be research to do; there’s still going to be advocacy work to do; but we’ll do that together.
TENC: We look very forward to doing exactly that together. Even within this landscape of limited expert care, how can patients access this type of specialty care today?
ML: A lot of people reach out to me on social media to ask this question. Both patients and physicians want to access this for their patients. So, if you are in a region that is close in proximity to someone who is doing this work – Hamilton, Vancouver, Ottawa – I would suggest reaching out to that person. Any gynaecologist can utilize the information provided from an advanced pelvic ultrasound as a tool to help manage a patient’s endo. And that is really one of the ways forward that I want to work in Canada. Basic pelvic ultrasound is not yet a part of our residency training, which is another limitation I am working to address.
For patients not located in those regions, travel is not ideal. You could speak with your physicians, your family doctor, your gynaecologist, about whether there are radiologists in your vicinity who are specialized in health issues like endometriosis. Let them know that these possibilities of advanced imaging are available, or possible at least, and ask how you can best find them in your region.
Discover more communication tips on advocating for expert care >
TENC: When it comes to endometriosis, what is your hope for the future and how can we get there?
ML: Let’s talk about hope for diagnosis first. I believe people can receive a diagnosis for endometriosis in different ways, I’m not sure it’s appropriate to say there’s an “only” way to diagnose endometriosis. There is perhaps a definitive way, but surgical diagnosis is not accessible or necessary for all patients. I would like to move towards a world where we have essentially five pillars through which endometriosis can be diagnosed.
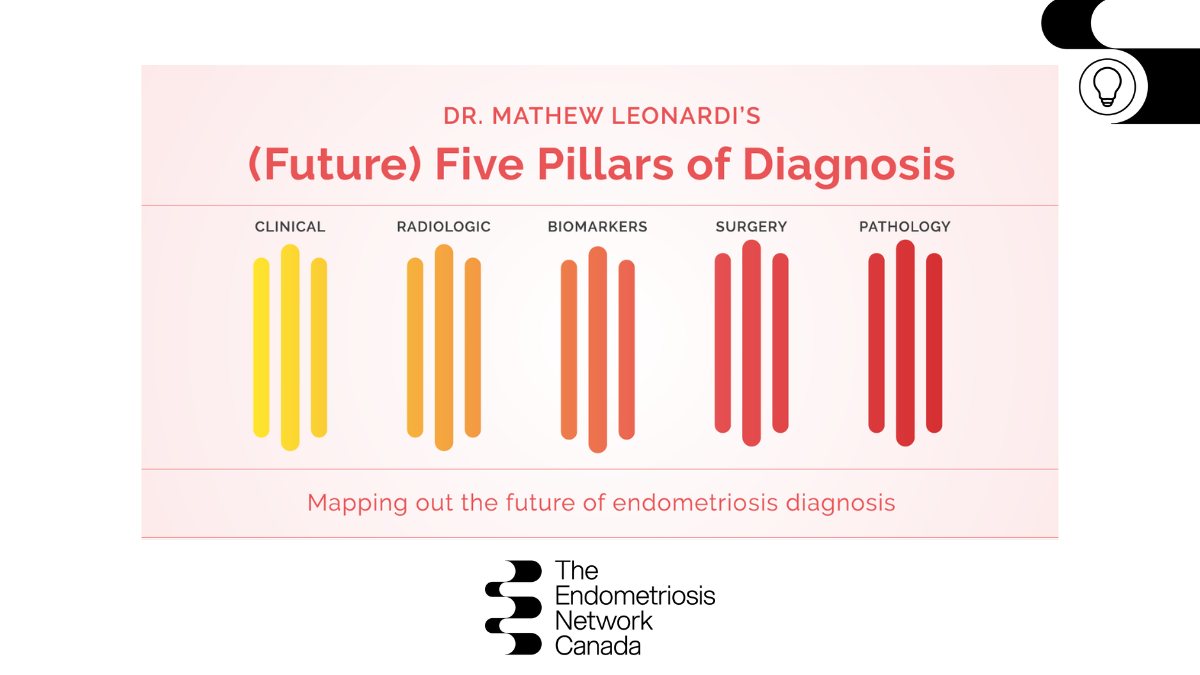
Pillar 1 – Clinical diagnosis
This is based on very clear, clinical evidence of the disease, such as a nodule visible on speculum examination, which is a classic sign of endometriosis. In the case of an umbilical (belly button) lesion that bleeds every month with your period, that is likely to lead to a clinical diagnosis.
Pillar 2 – Radiologic diagnosis
If endometriosis can be seen on imaging and all other options are eliminated – which, in the case of deep endometriosis, usually happens – this becomes a much less invasive approach to diagnosis than surgery.
Pillar 3 – Biomarkers
Biomarkers are either blood tests or other specimens such as a swab of the vagina, an endometrial biopsy, or even a salvia swab where we test for certain molecules that are present in that substance. This diagnostic tool is not yet available, but research is in progress at McMaster and around the world.
Pillar 4 – Surgery
This is the current standard for definitive diagnosis as it allows a surgeon to visually identify endometriosis and ideally excise. The ideal approach to diagnosis through surgery should include excision whenever possible.
Pillar 5 – Pathology
Once a sample of endometriosis tissue is obtained through surgery or a less invasive biopsy, it’s examined by a pathologist and tested to confirm the diagnosis.
Once a sample of endometriosis tissue is obtained through surgery or a less invasive biopsy, it’s examined by a pathologist and tested to confirm the diagnosis.
ML: For now, a final hope I have is that we start to consider endometriosis not as a single disease entity but as different disease entities depending on the subtype of endometriosis that is present.
We have not thought about refinement in our therapies for the symptoms that patients experience. We also haven’t considered how the various disease subtypes impact fertility and how the treatment of those various disease types impacts fertility treatment success.

This is an exciting opportunity because in just talking to hundreds of patients about endometriosis, I see how much of an impact it has beyond the pain. It affects quality of life, relationships, work, mental health, and more. Being able to know what you have and to have a good understanding of its severity, in my view, will start to take away some of that uncertainty, which is an important element of therapy.
Learn more about Dr. Leonardi, his research, work, and practice at: mathewleonardi.com
Connect with him on social:
Instagram – @drmathewleonardi
Twitter – @MathewLeonardi
Facebook – @drmathewleonardi
Stay tuned for the full-length video interview with more information for patients and clinicians — coming soon!